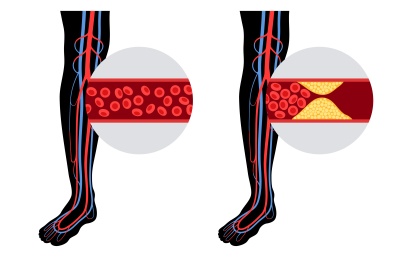
Peripheral artery disease (PAD) results from the build-up of plaque (atherosclerosis) in the arteries of the legs. For most people with PAD, symptoms may be mild or absent, and no treatment of the artery blockages is required. However as these blockages become more extensive, patients may experience pain and disability that limits their walking, and in the most advanced cases individuals may be at risk for loss of the limb unless circulation is improved. For these patients with severe PAD, attempts to improve blood flow in the leg are usually indicated. The goals of improving blood flow to the limb are to reduce pain, improve functional ability and quality of life, and to prevent amputation.
Currently, both minimally invasive treatments (such as angioplasty or stenting) and traditional procedures such as bypass surgery play important roles.
Determining the best procedure for an individual patient is a complex decision, based on the overall health of the patient, the history of their vascular problem and prior treatments, and the location and severity of the arterial blockages in the leg.
Catheter-based procedures such as angioplasty are less invasive but are also generally less durable, and have technical limitations when blockages are more extensive.
For patients who are not good candidates for angioplasty, or who have already failed a prior angioplasty attempt, lower extremity bypass surgery is a well-established and highly effective procedure. During these procedures, surgeons create an alternative conduit for blood flow to circumvent the area of blockage and restore direct flow to the lower leg and foot. This is a major surgical procedure performed under anesthesia via incisions in the leg. Careful assessment of the risks and benefits prior to surgery, as well as diligent medical, anesthetic, and surgical care, insures the best outcomes following leg bypass operations.
Like all surgical procedures, leg bypass surgery carries significant risks including heart attacks, blood clots, infections, and even death in 2 to 3 percent of patients. Patients with advanced PAD have a high frequency of significant heart disease, so a thorough evaluation for cardiac problems and a careful review of medical therapies is required prior to surgery.
The use of medications such as aspirin, blood pressure, and cholesterol-lowering drugs is critical before and after the operation. The other major complications are related to the leg itself, and include the risk of failure of the bypass and wound healing problems. Overall, bypass surgery is immediately successful in 90 to 95 percent of cases. The short and long-term success of the procedure is most closely linked to two factors: 1) the material employed for the bypass graft itself and 2) the quality of the arteries in the lower leg to which the graft is attached.
The best results are obtained by using a patient's own vein, the saphenous vein from the inside of the leg, to perform these grafts. When a good saphenous vein of sufficient length is not available, surgeons may choose to use other veins from the arm or leg, or to use an artificial (prosthetic) graft-however there is a fall-off in results for these alternatives. Therefore, an important consideration in selecting this procedure for a given patient is whether a good vein is likely to be available to perform the bypass.
Because blockages in the leg arteries extend over a considerable length, long incisions are often required, and various problems related to the healing of these wounds can occur in up to 20 percent of patients. These are often minor complications that may require dressings or antibiotics at home, but some can be more serious and lead to prolonged hospitalization or additional procedures.
Careful surgical technique and postoperative care are required to minimize these problems. In general, a vein bypass in the leg can be expected to last five years or longer in 60 to 70 percent of patients, although about one-quarter to one-third will require additional procedures to maintain the function of these grafts. Long-term follow-up, with regularly scheduled vascular examinations and ultrasound studies of the graft, is absolutely essential to achieve maximal benefit.
Abstinence from smoking and continued medical management including aspirin and cholesterol-lowering drugs is critical after surgery. Once recuperation is complete, patients who have had successful bypass surgery should expect to achieve relief of pain, improved healing of wounds on the foot, improved walking ability, and long-term freedom from amputation as long as the graft continues to function. For many patients with advanced PAD, lower extremity bypass surgery provides the most effective and most durable solution currently available.
Middle Georgia Vascular Surgery Center & Vein Solutions (MGVSC)
1025 N. Houston Rd
Warner Robins, GA 31093
Phone:
(478) 238-5513
Get Directions